You've Tried Everything. But Have You Been in Treatment?

We hear it all the time. It's practically the first thing a new client says when they sit down: "I've tried everything. Therapy, medication, you name it. Nothing works."
And I believe them. I believe they showed up. I believe they sat in the chair. I believe they tried.
But then I ask a few more questions. And here's what usually comes out:
"I went for a while, but it was mostly just talking."
"My therapist was really nice — like a friend, honestly."
"I'd go in, vent about my week, feel a little better, then go home and nothing really changed."
"I've been going for three years and I'm still dealing with the same stuff."
And there it is. Because here's the hard truth that nobody wants to say out loud: There's a massive difference between going to therapy and being in treatment.
The Best Friend Problem
Somewhere along the way, a lot of therapy became... comfortable. And I don't mean the good kind of comfortable — the kind where you feel safe enough to do hard work. I mean the kind where you walk in, talk about surface-level stuff, your therapist nods and validates, maybe offers a gentle reflection, and you leave feeling heard but not changed.
That's not treatment. That's a paid best friend.
And look — there's a time and place for support. There's value in being heard. But if you've been seeing someone for years and you're still stuck on the same issues, still triggered by the same things, still white-knuckling your way through the same patterns — the problem isn't you. The problem is that you were never actually in a treatment protocol.
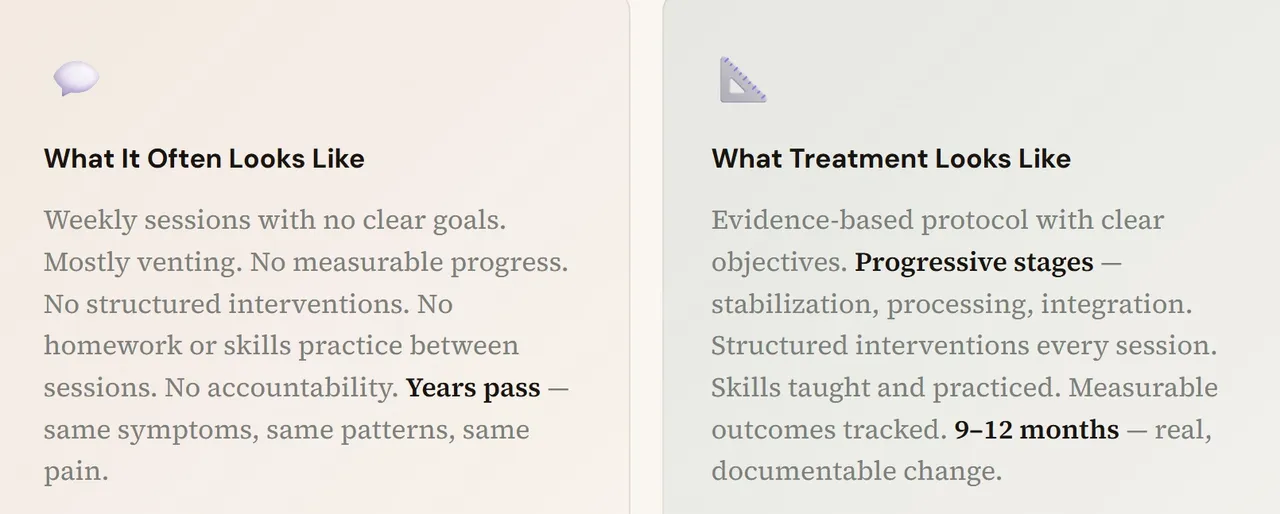

Therapy Is an Intervention — Not a Lifestyle
Here's something that might surprise you: you're not meant to be in therapy for the rest of your life.
Think about it this way. If you tore your ACL and went to physical therapy, you'd have a plan. Week 1 looks different from week 6 looks different from week 12. There are benchmarks. There's progression. There's a point where the PT says "You're strong enough now — go live your life and come back if you need a tune-up."
Nobody does physical therapy for five years for the same torn ACL. If they did, you'd say: something is wrong with the program.
Mental health treatment should work the same way. Evidence-based therapy has stages. It has a trajectory. It has an endpoint. You're supposed to move through it — not live in it.
Does life get heavy sometimes? Absolutely. Do you go back for a tune-up when a major stressor hits? Of course. But the core treatment — the work that rewires the patterns, processes the trauma, and builds the skills — that should have a beginning, a middle, and an end.
Why Nothing's Sticking
When clients tell me they've "tried everything," what I usually find is that they've tried a lot of versions of the same thing — unstructured talk therapy with different faces. And every time, they did the same thing: showed up, talked about the week, got some validation, went home. No one ever gave them a protocol. No one held them accountable. No one said "We're doing CPT for the next 12 weeks and here's what session 6 looks like."
That's throwing spaghetti at the wall. And of course nothing sticks — because spaghetti isn't a treatment plan.
Here's what it looks like when it works:
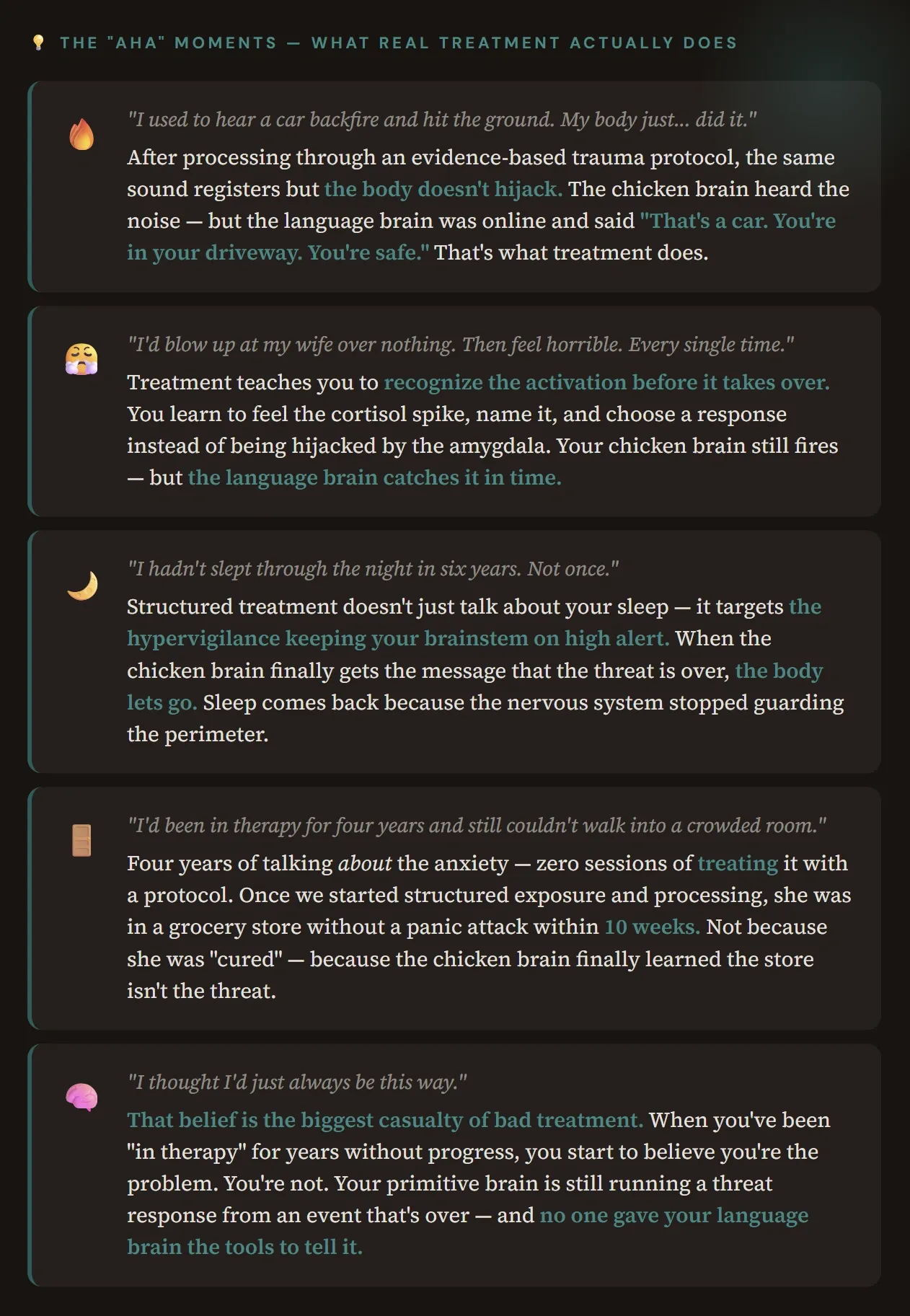
Every single one of these is the same mechanism: the chicken brain — your brainstem, your amygdala, your limbic system — is still running a survival program from a threat that has passed. Evidence-based treatment gives your language brain — your prefrontal cortex — the structure and the skills to reach the chicken brain and deliver the message: It's over. You're safe. You can stand down.
That's what therapy is supposed to do. Not talk about it forever. Resolve it.
How We Built Our Program
At Perkins PsyCare, we didn't build a talk-it-out practice. We built a therapeutic program — evidence-based, progressive, and time-bound — because that's what actually produces change.
Here's what it looks like when it works:

The whole program runs 9–12 months for the core treatment arc. Not because we picked an arbitrary number — because that's what the evidence says is needed for meaningful, lasting change in trauma, anxiety, depression, and complex psychological conditions. After that, maintenance therapy as needed.
You're coming to us for treatment. Not to gossip. Not to vent into a void. Not to sit in the same chair saying the same things to a new face every two years. You're coming to do the work — and our psychologists are going to hold you accountable to it, every single session.
The Hard Part Is the Point
I'm not going to lie to you — there will be sessions that are hard. There will be weeks where the last thing you want to do is show up. When life gets heavy, therapy can feel like one more thing on the list. One more obligation. One more place where you have to feel things you'd rather not feel.
That's actually the most important time to stay.
Because the moments when it's hardest to come in are usually the moments when the chicken brain is fighting the hardest to keep running its old program. It doesn't want to change. It's been doing this for years — maybe decades. And change feels dangerous to a system designed to avoid danger.
But if you push through — with structure, with accountability, with a provider who isn't going to let you float through surface-level sessions — that's when the real shift happens. That's when the nightmares quiet down. That's when the triggers lose their grip. That's when you stop surviving and start living.
And eventually, you graduate. Not because we gave up on you — because you don't need us anymore. And that's the whole point. - Dr. Monika Diaz, PhD
Enjoyed this article?
Get notified when we publish new insights.
